37 6.5 Problems Facing Older Americans
Learning Objectives
- Present a brief sociodemographic profile of the US elderly.
- Discuss the several problems experienced by the US elderly.
- Describe how the social attitudes of older Americans generally differ from those of younger Americans.
We now turn our attention to older people in the United States. We first sketch a demographic profile of our elderly and then examine some of the problems they face because of their age and because of ageism.
Who Are the Elderly?
Table 6.2 “Demographic Composition of the Elderly, 2010” presents the demographic composition of Americans aged 65 or older. Slightly more than half the elderly are 65–74 years of age, and about 57 percent are female, reflecting males’ shorter life spans as discussed earlier. About 80 percent of the elderly are non-Latino whites, compared to about 66 percent in the population as a whole; 8.6 percent are African American, compared to about 13 percent of the population; and 7.0 percent are Latino, compared to 15 percent of the population. The greater proportion of whites among the elderly and lower proportions of African Americans and Latinos reflects these groups’ life expectancy differences discussed earlier and also their differences in birth rates.
Table 6.2 Demographic Composition of the Elderly, 2010
| Age | |
| 65–74 years | 52.3% |
| 75–84 years | 33.4% |
| 85 years and over | 14.3% |
| Gender | |
| Female | 56.9% |
| Male | 43.1% |
| Race and/or ethnicity* | |
| White, non-Latino | 80.1% |
| African American | 8.6% |
| Latino | 7.0% |
| Asian/Pacific Islander | 3.5% |
| Amer. Ind., Esk., Aleut. | 0.6% |
| Two or more races | 0.7% |
| Living in poverty | 9.0% |
| Marital status | |
| Married | 57.6% |
| Widowed | 28.1% |
| Divorced | 10.0% |
| Never married | 4.3% |
| Years of school completed | |
| 0–8 years | 10.2% |
| 1–3 years of high school | 10.3% |
| High school graduate | 36.4% |
| 1–3 years of college | 20.6% |
| College graduate | 22.5% |
| Labor force participation | |
| Employed | 16.2% |
| Unemployed | 1.2% |
| Not in labor force | 82.6% |
| Household income* | |
| Under $15,000 | 18.8% |
| $15,000–$24,999 | 20.7% |
| $25,000–$34,999 | 15.4% |
| $35,000–49,999 | 15.1% |
| $50,000–$74,999 | 14.2% |
| $75,000–$99,999 | 6.5% |
| $100,000 and over | 9.4% |
| * 2009 data | |
|---|---|
Source: Data from US Census Bureau. (2012). Statistical abstract of the United States: 2012. Washington, DC: US Government Printing Office. Retrieved from http://www.census.gov/compendia/statab.

The lower proportions of African Americans and Latinos among the elderly partly reflect these groups’ lower life expectancies.
Evgeni Zotov – Grandparents – CC BY-NC-ND 2.0.
The percentage of elders living in poverty is 9.0, compared to 15.1 percent of the entire population. Although most elders have fixed incomes, the fact that their family size is usually one or two means that they are less likely than younger people to live in poverty. In fact, today’s elderly are financially much better off than their grandparents were, thanks to Social Security, Medicare (the federal health insurance program for older Americans), pensions, and their own assets. We will revisit the health and financial security of elders a little later.
Turning to education, about 22 percent of the elderly are college graduates, compared to about 29 percent of the population as a whole. This difference reflects the fact that few people went to college when today’s elderly were in their late teens and early twenties. However, it is still true that today’s elders are better educated than any previous generation of elders. Future generations of the elderly will be even better educated than those now.
While most elders are retired and no longer in the labor force, about 16 percent do continue to work (see Table 6.2 “Demographic Composition of the Elderly, 2010”). These seniors tend to be in good health and to find their jobs psychologically satisfying. Compared to younger workers, they miss fewer days of work for health or other reasons and are less likely to quit their jobs for other opportunities (Sears, 2009).
Although we emphasized earlier that many older Americans do not fit the negative image with which they are portrayed, it is still true that they face special problems because of their age and life circumstances and because of ageism. We discuss some of these here.
Physical and Mental Health
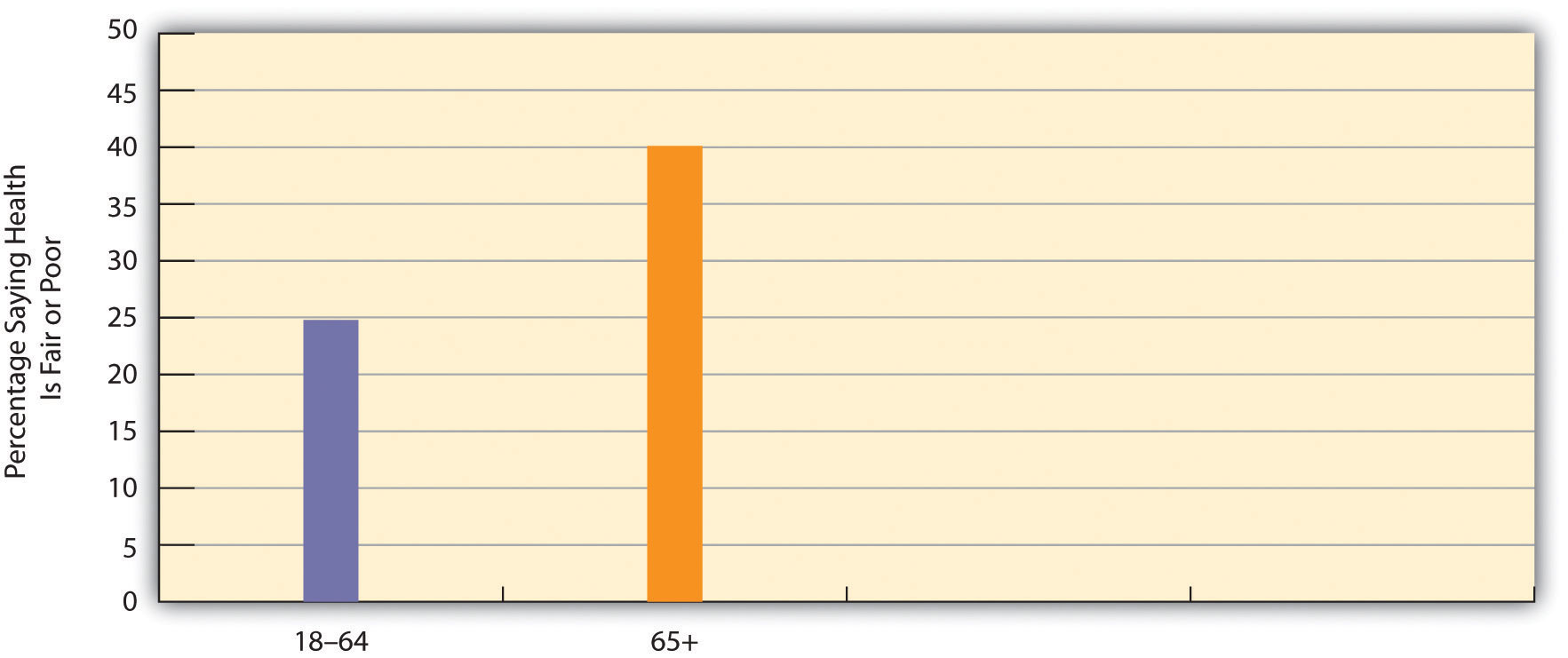
Perhaps the problem that comes most readily to mind is health, or, to be more precise, poor health. It is true that many older people remain in good health and are fully able to function mentally and physically (Rowe et al., 2010). Still, the biological and psychological effects of aging do lead to greater physical and mental health problems among the elderly than in younger age groups, as we briefly discussed earlier. These problems are reflected in responses to the General Social Survey (GSS) question, “Would you say your own health, in general, is excellent, good, fair, or poor?” Figure 6.6 “Age and Self-Reported Health” shows that the elderly are more likely than the nonelderly to report that their health is only fair or poor.
Figure 6.6 Age and Self-Reported Health
Source: Data from General Social Survey. (2010). Retrieved from http://sda.berkeley.edu/cgi-bin/hsda?harcsda+gss10.
The elderly’s perception of their own health is supported by government estimates of chronic health conditions for older Americans. Of all people aged 65 or older not living in a nursing home or other institution, almost 50 percent have arthritis, 56 percent have high blood pressure, 32 percent have heart disease, 35 percent have hearing loss, 18 percent have vision problems, and 19 percent have diabetes (these numbers add up to more than 100 percent as people may have several health conditions) (Federal Interagency Forum on Aging-Related Statistics, 2010). These rates are much higher than those for younger age groups.
The elderly also suffer from dementia, including Alzheimer’s disease, which affects almost 13 percent of people 65 or older (Alzheimer’s Association, 2009). Another mental health problem is depression, which affects almost 15 percent of people 65 or older. Because of mental or physical disability, about two-thirds of all people 65 or older need help with at least one “daily living” activity, such as preparing a meal (Federal Interagency Forum on Aging-Related Statistics, 2010).

Older people visit the doctor and hospital more often than younger people. Partly for this reason, adequate health care for the elderly is of major importance.
Ted Van Pelt – The Coopers – CC BY 2.0.
If the elderly have more health problems, then adequate care for them is of major importance. They visit the doctor and hospital more often than their middle-aged counterparts. Medicare covers about one-half of their health-care costs; this is a substantial amount of coverage but still forces many seniors to pay thousands of dollars annually themselves. Some physicians and other health-care providers do not accept Medicare “assignment,” meaning that the patient must pay an even higher amount. Moreover, Medicare pays little or nothing for long-term care in nursing homes and other institutions and for mental health services. All these factors mean that older Americans can still face high medical expenses or at least pay high premiums for private health insurance.
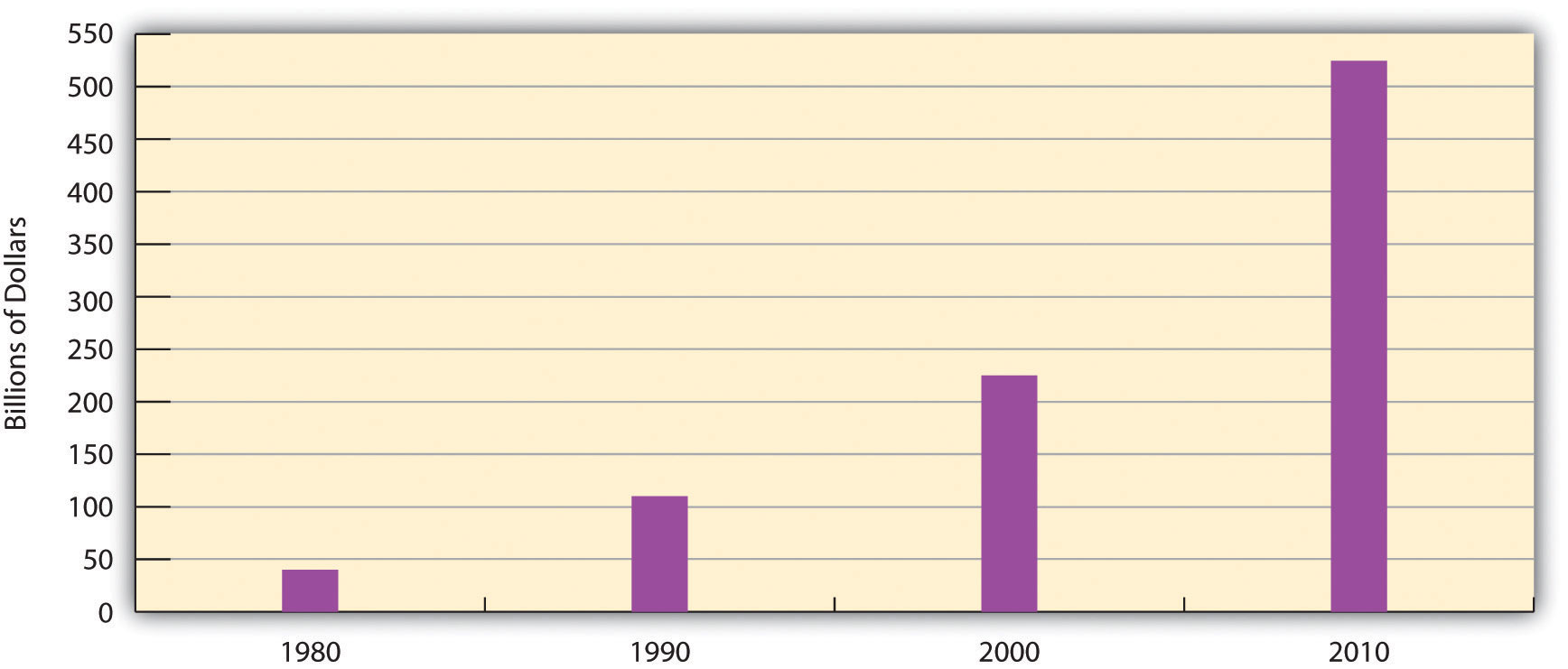
In addition, Medicare costs have risen rapidly along with other health-care costs. Medicare expenditures soared from about $37 billion in 1980 to more than $500 billion today (see Figure 6.7 “Medicare Expenditures, 1980–2010”). As the population continues to age and as health-care costs continue to rise, Medicare expenses will continue to rise as well, making it increasingly difficult to find the money to finance Medicare.
Figure 6.7 Medicare Expenditures, 1980–2010
Source: Data from Centers for Medicare and Medicaid Services. (n.d.). National health expenditure data. Retrieved from http://www.hhs.gov.
Nursing Home Care
While most older Americans live by themselves or with their families, a small minority live in group settings. A growing type of group setting is the continuous care retirement community, a setting of private rooms, apartments, and/or condominiums that offers medical and practical care to those who need it. In some such communities, residents eat their meals together, while in others they cook for themselves. Usually these communities offer above-average recreational facilities and can be very expensive, as some require a lifetime contract or at least monthly fees that can run into the thousands of dollars.

Nursing homes are often understaffed to save costs and are also generally not subject to outside inspection. These conditions help contribute to the neglect of nursing home residents.
Sheila – Christian Nursing Home – CC BY-NC-ND 2.0.
For elders who need high-level medical care or practical support, nursing homes are the primary option. About 16,100 nursing homes exist, and 3.9 percent of Americans 65 or older live in them (Federal Interagency Forum on Aging-Related Statistics, 2010). About three-fourths of all nursing home residents are women. Almost all residents receive assistance in bathing and showering, 80 percent receive help in using the bathroom, and one-third receive help in eating.
As noted earlier, Medicare does not pay for long-term institutional care for most older Americans. Because nursing home care costs at least $70,000 yearly, residents can quickly use up all their assets and then, ironically, become eligible for payments from Medicaid, the federal insurance program for people with low incomes.
If one problem of nursing homes is their expense, another problem is the quality of care they provide. Because their residents are typically in poor physical and/or mental health, their care must be the best possible, as they can do little to help themselves if their care is substandard. As more people enter nursing homes in the years ahead, the quality of nursing home care will become even more important. Yet there is much evidence that nursing home care is often substandard and is replete with neglect and abuse (DeHart, Webb, & Cornman, 2009).
Financial Security and Employment
Earlier we noted that the elderly are less likely than younger age groups to live in poverty and that their financial status is much better than that of previous generations of older people. One reason for this is Social Security: If Social Security did not exist, the poverty rate of the elderly would be 45 percent, or five times higher than the actual rate (Kerby, 2012). Without Social Security, then, nearly half of all people 65 or older would be living in official poverty, and this rate would be even much higher for older women and older persons of color. However, this brief summary of their economic well-being obscures some underlying problems (Carr, 2010; Crawthorne, 2008).
First, recall Chapter 2 “Poverty”’s discussion of episodic poverty, which refers to the drifting of many people into and out of poverty as their jobs and other circumstances change. Once they become poor, older people are more likely than younger ones to stay poor, as younger people have more job and other opportunities to move out of poverty. Recall also that the official poverty rate obscures the fact that many people live just above it and are “near poor.” This is especially true of the elderly, who, if hit by large medical bills or other expenses, can hardly afford to pay them.
Second, the extent of older Americans’ poverty varies by sociodemographic factors and is much worse for some groups than for others (Carr, 2010). Older women, for example, are more likely than older men to live in poverty for at least two reasons. Because women earn less than men and are more likely to take time off from work during their careers, they have lower monthly Social Security benefits than men and smaller pensions from their employers. As well, women outlive men and thus use up their savings. Racial and ethnic disparities also exist among the elderly, reflecting poverty disparities in the entire population, as older people of color are much more likely than older whites to live in poverty (Carr, 2010). Among women 65 and older, 9 percent of whites live in poverty, compared to 27 percent of African Americans, 12 percent of Asians, and 21 percent of Hispanics.

Older women are more likely than older men to live in poverty.
Christian Haugen – Old woman feeding the pigeon – CC BY 2.0.
Third, monthly Social Security benefits are tied to people’s earnings before retirement; the higher the earnings, the higher the monthly benefit. Thus a paradox occurs: People who earn low wages will get lower Social Security benefits after they retire, even though they need higher benefits to make up for their lower earnings. In this manner, the income inequality that exists before retirement continues to exist after it.
This paradox reflects a wider problem involving Social Security. However helpful it might be in aiding older Americans, the aid it provides lags far behind comparable programs in other wealthy Western nations (see Note 6.27 “Lessons from Other Societies”). Social Security payments are low enough that almost one-third of the elderly who receive no other income assistance live in official poverty. For all these reasons, Social Security is certainly beneficial for many older Americans, but it remains inadequate compared to what other nations provide.
Lessons from Other Societies
Aging Policy and Programs in the Netherlands and Sweden
A few years ago, AARP assessed quality-of-life issues for older people and the larger society in sixteen wealthy democracies (the nations of North America and Western Europe, along with Australia and Japan). Each nation was rated (on a scale of 1–5, with 5 being the highest score) on seventeen criteria, including life expectancy, health care for the elderly, pension coverage, and age-discrimination laws. Of the sixteen nations, the Netherlands ranked first, with a total score of 64, while Italy ranked last, with a score of 48; the United States was thirteenth, with a score of 50. Despite its immense wealth, then, the United States lagged behind most other democracies. Because a “perfect” score would have been 85 (17 × 5), even the Netherlands fell short of an ideal quality of life as measured by the AARP indicators.
Why did the United States not rank higher? The experience of the Netherlands and Sweden, both of which have longer life expectancies than the United States, points to some possible answers. In the Netherlands, everyone at age 65 receives a full pension that does not depend on how much money they earned while they were working, and everyone thus gets the same amount. This amount is larger than the average American gets, because Social Security does depend on earnings and many people earned fairly low amounts during their working years. As a result, Dutch elderly are much less likely than their American counterparts to be poor. The Dutch elderly (and also the nonelderly) have generous government insurance for medical problems and for nursing home care; this financial help is much higher than older Americans obtain through Medicare.
As one example, the AARP article mentioned an elderly Dutch woman who had cancer surgery and thirty-two chemotherapy treatments, for which she paid nothing. In the United States, the chemotherapy treatments would have cost at least $30,000. Medicare would have covered only 80 percent of this amount, leaving a patient to pay $6,000.
The Netherlands also helps its elderly in other ways. One example is that about one-fourth of that nation’s elderly receive regular government-subsidized home visits by health-care professionals and/or housekeepers; this practice enables the elderly to remain independent and avoid having to enter a nursing home. In another example, the elderly also receive seven days of free riding on the nation’s rail system.
Sweden has a home-care visitation program that is similar to the Netherlands’ program. Many elderly are visited twice a day by a care assistant who helps them bathe and dress in the morning and go to bed at night. The care assistant also regularly cleans their residence and takes them out for exercise. The Swedish government pays about 80 percent of the costs of this assistance and subsidizes the remaining cost for elderly who cannot afford it. Like the Netherlands’ program, Sweden’s program helps the elderly to remain independent and live at home rather than enter a nursing institution.
Compared to the United States, then, other democracies generally provide their elderly less expensive or free health care, greater financial support during their retirement, and home visits by health-care professionals and other assistants. In these and other ways, these other governments encourage “active aging.” Adoption of similar policies in the United States would improve the lives of older Americans and perhaps prolong their life spans.
Sources: Edwards, 2004; Hartlapp & Schmid, 2008; Ney, 2005

Older people who want to work may have trouble finding employment because of age discrimination and other factors.
Wikimedia Commons – CC BY 2.0.
Workplace Ageism
Older Americans also face problems in employment. Recall that about 16 percent of seniors remain employed. Other elders may wish to work but are retired or unemployed because several obstacles make it difficult for them to find jobs. First, many workplaces do not permit the part-time working arrangements that many seniors favor. Second, and as the opening news story indicated, the rise in high-tech jobs means that older workers would need to be retrained for many of today’s jobs, and few retraining programs exist. Third, although federal law prohibits age discrimination in employment, it exists anyway, as employers do not think older people are “up to” the job, even though the evidence indicates they are good, productive workers (Berger, 2009; Roscigno, 2010). Finally, earnings above a certain level reduce Social Security benefits before full retirement age, leading some older people to avoid working at all or to at least limit their hours. All these obstacles lead seniors to drop out of the labor force or to remain unemployed (Gallo, Brand, Teng, Leo-Summers, & Byers, 2009).
Age discrimination in the workplace merits some further discussion. According to sociologist Vincent J. Roscigno (2010), survey evidence suggests that more than half of older workers have experienced or observed age discrimination in the workplace, and more than 80 percent of older workers have experienced or observed jokes, disrespect, or other prejudicial comments about old age. Roscigno notes that workplace ageism receives little news media attention and has also been neglected by social scientists. This is so despite the related facts that ageism in the workplace is common and that the older people who experience this discrimination suffer financial loss and emotional problems. Roscigno (2010, p. 17) interviewed several victims of age discrimination and later wrote, “Many conveyed fear of defaulting on mortgages or being unable to pay for their children’s college after being pushed out of their jobs. Others expressed anger and insecurity over the loss of affordable health insurance or pension benefits…Just as prevalent and somewhat surprising to me in these discussions were the less-tangible, yet deeper social-psychological and emotional costs that social science research has established for racial discrimination or sexual harassment, for instance, but are only now being considered in relation to older workers.”
One of the people Roscigno interviewed was a maintenance worker who was laid off after more than two decades of working for his employer. This worker was both hurt and angry. “They now don’t want to pay me my pension,” he said. “I was a good worker for them and always did everything they asked. I went out of my way to help train people and make everything run smoothly, so everybody was happy and it was a good place to work. And now this is what I get, like I never really mattered to them. It’s just not right” (Roscigno, 2010, p. 17).
Bereavement and Social Isolation
“We all need someone we can lean on,” as a famous Rolling Stones song goes. Most older Americans do have adequate social support networks, which, as we saw earlier, are important for their well-being. However, a significant minority of elders live alone and do not see friends and relatives as often as they wish. Bereavement takes a toll, as elders who might have been married for many years suddenly find themselves living alone. Here a gender difference again exists. Because women outlive men and are generally younger than their husbands, they are three times more likely than men (42 percent compared to 13 percent) to be widowed and thus much more likely to live alone (see Table 6.3 “Living Arrangements of Noninstitutionalized Older Americans, 2010”).
Table 6.3 Living Arrangements of Noninstitutionalized Older Americans, 2010
| Men (%) | Women (%) | |
|---|---|---|
| Living alone | 19 | 41 |
| Living with spouse | 70 | 37 |
| Other arrangement | 11 | 21 |
Source: Data from Administration on Aging. (2011). A profile of older Americans: 2011. Retrieved from http://www.aoa.gov/aoaroot/aging_statistics/Profile/2011/docs/2011profile.pdf.
Many elders have at least one adult child living within driving distance, and such children are an invaluable resource. At the same time, however, some elders have no children, because either they have outlived their children or they never had any. As baby boomers begin reaching their older years, more of them will have no children because they were more likely than previous generations to not marry and/or to not have children if they did marry. Baby boomers thus face a relative lack of children to help them when they enter their “old-old” years (Leland, 2010).
Bereavement is always a difficult experience, but because so many elders lose a spouse, it is a particular problem in their lives. The grief that usually follows bereavement can last several years and, if it becomes extreme, can involve anxiety, depression, guilt, loneliness, and other problems. Of all these problems, loneliness is perhaps the most common and the most difficult to overcome.
Elder Abuse
Some seniors fall prey to their own relatives who commit elder abuse against them. Such abuse involves one or more of the following: physical or sexual violence, psychological or emotional abuse, neglect of care, or financial exploitation (Novak, 2012). Accurate data are hard to come by since few elders report their abuse, but estimates say that at least 10 percent of older Americans have suffered at least one form of abuse, amounting to hundreds of thousands of cases annually. However, few of these cases come to the attention of the police or other authorities (National Center on Elder Abuse, 2010).
Although we may never know the actual extent of elder abuse, it poses a serious health problem for the elders who are physically, sexually, and/or psychologically abused or neglected, and it may even raise their chances of dying. One study of more than 2,800 elders found that those who were abused or neglected were three times more likely than those who were not mistreated to die during the next thirteen years. This difference was found even after injury and chronic illness were taken into account (Horn, 1998).
A major reason for elder abuse seems to be stress. The adult children and other relatives who care for elders often find it an exhausting, emotionally trying experience, especially if the person they are helping needs extensive help with daily activities. Faced with this stress, elders’ caregivers can easily snap and take out their frustrations with physical violence, emotional abuse, or neglect of care.
Senior Power: Older Americans as a Political Force
Older Americans often hold strong views on issues that affect them directly, such as Medicare and Social Security. In turn, politicians often work to win the older vote and shape their political stances accordingly.

During the past few decades, older people have become more active politically on their own behalf.
Marc Nozell – Bernie Sanders – CC BY-NC 2.0.
To help address all the problems discussed in the preceding pages, several organizations have been established since the 1980s to act as interest groups in the political arena on behalf of older Americans (Walker, 2006). One of the most influential groups is the American Association of Retired Persons (AARP), which is open to people 50 or older. AARP provides travel and other discounts to its members and lobbies Congress and other groups extensively on elderly issues. Its membership numbers about 40 million, or 40 percent of the over-50 population. Some critics say AARP focuses too much on its largely middle-class membership’s self-interests instead of working for more far-reaching economic changes that might benefit the older poor; others say its efforts on Medicare, Social Security, and other issues do benefit the elderly from all walks of life. This controversy aside, AARP is an influential force in the political arena because of its numbers and resources.
A very different type of political organization of the elderly was the Gray Panthers, founded by the late Maggie Kuhn in 1970 (Kuhn, Long, & Quinn, 1991). Although this group has been less newsworthy since Kuhn’s death in 1995, at its height it had some eighty-five local chapters across the nation and 70,000 members and supporters. A more activist organization than AARP and other lobbying groups for the elderly, the Gray Panthers took more liberal stances. For example, it urged the establishment of a national health-care service and programs to increase affordable housing for the elderly.
As older Americans have engaged the political process on their own behalf, critics have charged that programs for the elderly are too costly to the nation, that the elderly are better off than groups like AARP claim, and that new programs for the elderly will take even more money from younger generations and leave them insufficient funds for their own retirement many years from now. Their criticism, which began during the 1980s, is termed the generational equity argument (Williamson, McNamara, & Howling, 2003).
Advocates for the elderly say the generational equity critics exaggerate the financial well-being of older Americans and neglect the fact that many older Americans, especially women and those of color, are poor or near poor and thus need additional government aid. Anything we can do now to help the aged, they continue, will also help future generations of the elderly. As Lenard W. Kaye (1994, p. 346) observed in an early critique of the generational equity movement, “In the long run, all of us can expect to live into extended old age, barring an unexpected fatal illness or accident. To do injustice to our current generation of elders, by means of policy change, can only come back to haunt us as each and every one of us—children, young families, and working people—move toward the latter stages of the life course.”
People Making a Difference
College Students Helping Senior Citizens
After Hurricane Irene swept up the East Coast in August 2011, many towns and cities faced severe flooding. One of these towns was Cranford, New Jersey, just southwest of Newark. Streets and hundreds of homes flooded, and many residents’ belongings were ruined.
Union County College, which has campuses in Cranford and a few other towns, came to Cranford residents’ aid. As the college president explained in late August, “Many of the town’s residents are senior citizens. Even though the fall term won’t begin until Sept. 1, we’ve still got a number of strong men and women on campus to help residents clear out their basements and help move whatever people needed moved.”
Led by the dean of college life, a dozen or so students went house-to-house on a Cranford street that experienced the worst flooding to aid the town’s senior citizens and younger ones as well. The dean later recalled, “Everyone we met was just so happy to see us there helping out. Sometimes they had plenty of work for us. Other times, they just smiled and said they were glad to know we cared.”
A news report summarized the impact of the students’ assistance: “In the coming weeks and months, Cranford residents will be able to recover what their town lost to Irene. But they may never forget the damage Irene caused, nor are they likely to forget how Union County College’s students came to help them in their time of need.” At a time of crisis, the staff and students of Union County College in the small town of Cranford, New Jersey, made a big difference in the lives of Cranford’s senior citizens and younger residents alike.
Source: Cranford Chronicle, 2011
Key Takeaways
- The US elderly experience several health problems, including arthritis, high blood pressure, heart disease, hearing loss, vision problems, diabetes, and dementia.
- Nursing home care in the United States is very expensive and often substandard; neglect and abuse of nursing home residents is fairly common.
- Despite help from Social Security, many older Americans face problems of financial security.
- It is difficult to determine the actual extent of elder abuse, but elder abuse often has serious consequences for the health and lives of older Americans.
- During the last few decades, older Americans have been active in the political process on their own behalf and today are an important political force in the United States.
For Your Review
- What do you think is the worst or most serious problem facing the US elderly? Explain your answer.
- The text suggests that the lives of the US elderly would be improved if the United States were to adopt some of the policies and practices that other nations have for their elderly. Explain why you agree or disagree with this suggestion.
References
Alzheimer’s Association. (2009). 2009 Alzheimer’s disease facts and figures. Chicago, IL: Author.
Berger, E. D. (2009). Managing age discrimination: An examination of the techniques used when seeking employment. The Gerontologist, 49(3), 317–332.
Carr, D. (2010). Golden years? Poverty among older Americans. Contexts, 9(1), 62–63.
Cranford Chronicle. (2011, August 31). County College students help Cranford residents cleanup. Cranford Chronicle. Retrieved from http://www.nj.com/cranford/index.ssf/2011/2008/county_college_students_help_c.html.
Crawthorne, A. (2008). Elderly poverty: The challenge before us. Washington, DC: Center for American Progress.
DeHart, D., Webb, J., & Cornman, C. (2009). Prevention of elder mistreatment in nursing homes: Competencies for direct-care staff. Journal of Elder Abuse & Neglect, 21(4), 360–378.
Edwards, M. (2007). As Good As It Gets: What Country Takes the Best Care of Its Older Citizens? In D. S. Eitzen (Ed.), Solutions to Social Problems: Lessons from Other Societies (4th ed., pp. 76–85). Boston, MA: Allyn & Bacon.
Federal Interagency Forum on Aging-Related Statistics. (2010). Older Americans 2010: Key indicators of well-being. Washington, DC: US Goverment Printing Office.
Gallo, W. T., Brand, J. E., Teng, H.-M., Leo-Summers, L., & Byers, A. L. (2009). Differential impact of involuntary job loss on physical disability among older workers: Does predisposition matter? Research on Aging, 31(3), 345–360.
Hartlapp, M., & Schmid, G. (2008). Labour market policy for “active ageing” in Europe: Expanding the options for retirement transitions. Journal of Social Policy, 37(3), 409–431.
Horn, D. (1998, August 17). Bad news on elder abuse. Time, p. 82.
Kaye, L. W. (1994). Generational equity: Pitting young against old. In J. Robert B. Enright (Ed.), Perspectives in social gerontology (pp. 343–347). Boston, MA: Allyn and Bacon.
Kerby, S. (2012). Debunking poverty myths and racial stereotypes. Washington, DC: Center for American Progress.
Kuhn, M., Long, C., & Quinn, L. (1991). No stone unturned: The life and times of Maggie Kuhn. New York, NY: Ballantine Books.
Leland, J. (2010, April 25). A graying population, a graying work force. New York Times, p. A14.
National Center on Elder Abuse. (2010). Why should I care about elder abuse? Washington, DC: Author.
Ney, S. (2005). Active aging policy in Europe: Between path dependency and path departure. Ageing International, 30, 325–342.
Novak, M. (2012). Issues in aging (3rd ed.). Upper Saddle River, NJ: Pearson.
Roscigno, V. J. (2010). Ageism in the American workplace. Contexts, 9(1), 16–21.
Rowe, J. W., Berkman, L. F., Binstock, R., Boersch-Supan, A., Cacioppo, J., Carsternsen, L., et al. (2010). Policies and politics for an aging America. Contexts, 9(1), 22–27.
Sears, D. (2009, September 6). Myths busted on older workers’ job performance. TheLadders. Retrieved from http://www.career-line.com/job-search-news/myths-busted-on-older-workers-job-performance/.
Walker, A. (2006). Aging and politics: An international perspective. In R. H. Binstock & L. K. George (Eds.), Handbook of aging and the social sciences (6th ed., pp. 338–358). New York, NY: Academic Press.
Williamson, J. B., McNamara, T. K., & Howling, S. A. (2003). Generational equity, generational interdependence, and the framing of the debate over social security reform. Journal of Sociology and Social Welfare, 30(3), 3–14.